It may be advisable to do surgery at a later age and use a 3-piece intraocular lens.
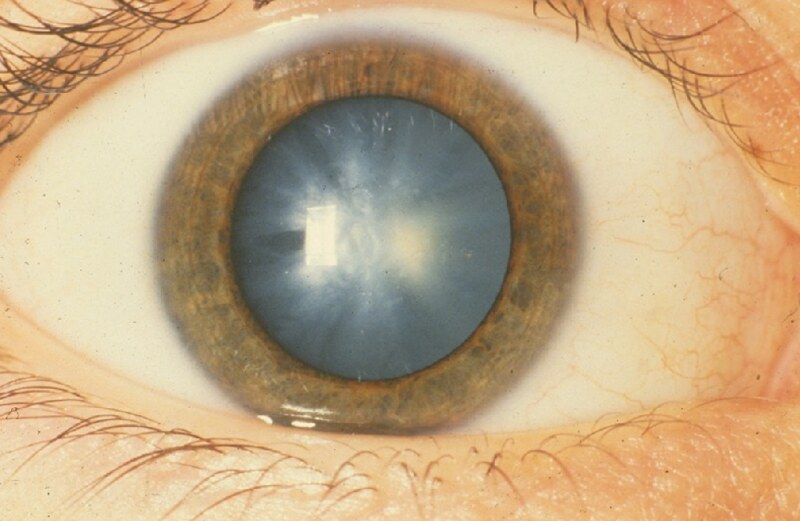
Congenital cataracts may be bilateral or unilateral, progressive or not, and may or may not cause significant visual impairment. Common causes are metabolic and genetic syndromes (e.g. Down’s syndrome) and infections (e.g. congenital rubella). (Image source)
Congenital and infantile cataracts are one of the leading causes of blindness in childhood. This was traditionally managed by cataract surgery and early intraocular lens (IOL) implantation. However, previous studies have shown that this treatment does not confer any visual benefit, with the additional risk of extra procedures to remove visual axis opacities (VAO). The VAO is a result of either the proliferation of the remaining lens cells or products of inflammation. The use of aphakic glasses or lenses, which is another option, is hindered by access to optometric care, utility (glasses can be heavy!), and ability of the family and care providers to manage lens insertion and removal.
In this population-based, prospective cohort study, 105 children were recruited through a national clinic network. These children (total, 162 eyes) had primary IOL implantation within the first 2 years of life. The objective of this study was to look for VAO predictors in this sample, evaluating the effect of factors such as age, axial length, socio-economic status, IOL model, and postoperative steroid use.
Results showed that VAO occurred in almost half of the eyes (45%) within the first year after cataract surgery. Of the factors evaluated, the use of a 3-piece IOL and a greater age at surgery were demonstrated to be independently protective against VAO. The inflammatory type of VAO was also shown to be independently associated with a lower socioeconomic status.
The findings of this study may be useful as additional guidelines in the management of congenital and infantile cataracts.
Solebo, A., & Rahi, J. (2020). Visual Axis Opacity after Intraocular Lens Implantation in Children in the First 2 Years of Life. Ophthalmology. https://doi.org/10.1016/j.ophtha.2020.02.038