The results of this study show that in patients with myopia and normal tension glaucoma, the way the disc is tilted may influence visual field progression.
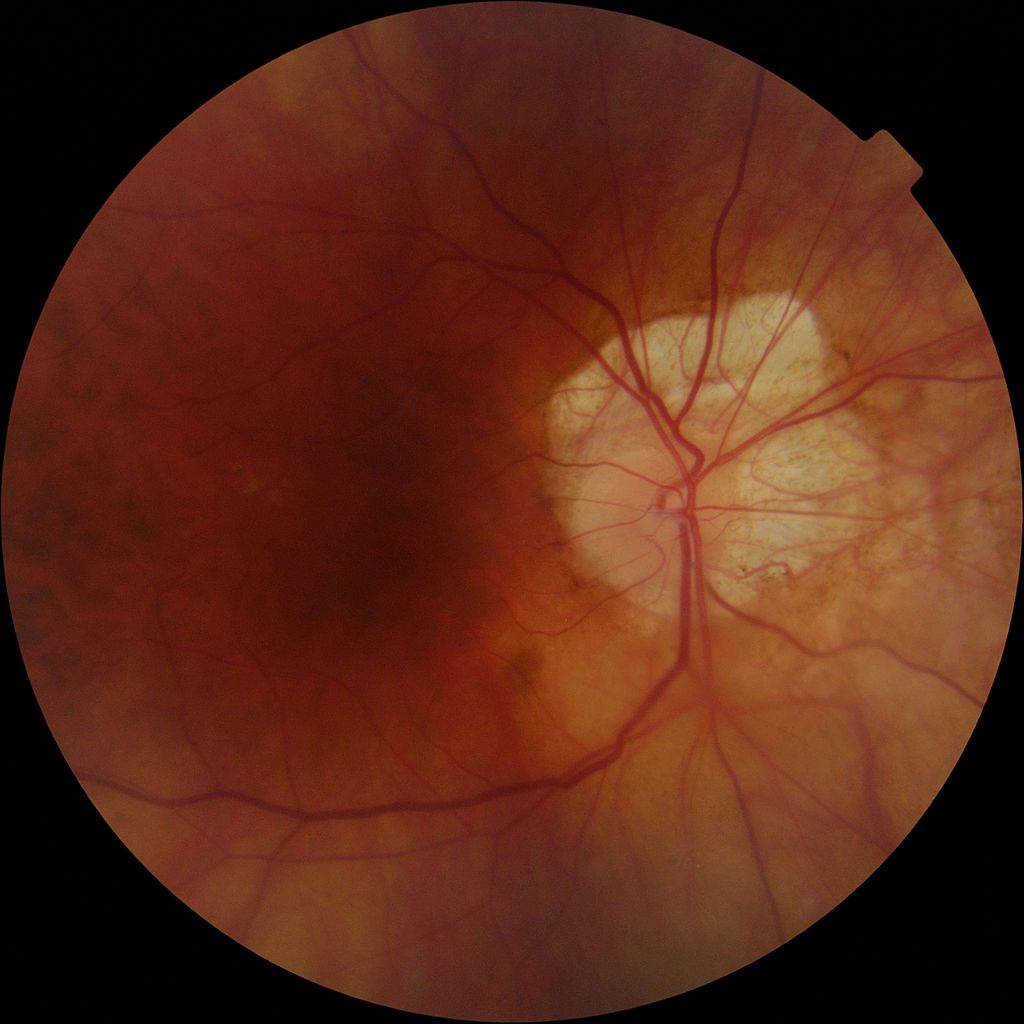
Fundus photo showing a large myopic crescent in right eye with peripapillary choroidal atrophy. (Source via CC-by SA 3.0)
Myopia has been known as a risk factor for glaucoma, as reported in previous studies. However, the cache of evidence presents different results regarding the role of myopia in the progression of glaucoma. Some have suggested that optic nerve head (ONH) morphology, such as a tilted disc or peripapillary atrophy (PPA), contribute to the worsening of this disease. On the other hand, other studies have shown no association between ONH deformation and glaucoma progression.
The differences in the results of these studies were due to the lack of methodology standardization and/or stratified analysis according to intraocular pressure (IOP) measurements and glaucoma medications.
In this retrospective longitudinal study, patients with normal tension glaucoma (NTG) and myopia who did not use IOP-lowering medications until glaucomatous visual field (VF) progression was documented were enrolled. This way, the natural course of the disease in this subset of patients could be monitored.
A total of 97 eyes in 97 patients were included in the study. Only 33% (32) showed disease progression over the course of 3 years. The factors associated with VF progression in these patients with untreated NTG and myopia were the following: a younger age, disc hemorrhage, less disc tilt direction, and less PPA direction. VF progression was observed at an average of 55 months after diagnosis, with the patients an average of 52 years old. There were no significant differences between the initial and final VF defect patterns and in the presence of a paracentral scotoma between the two outcomes (with and without progression).
Compared to previous literature, NTG with myopia was found in this study to be less associated with VF progression. However, in terms of disc tilt, the study found that, using the Kaplan-Meier survival curve, patients in which the disc was temporally tilted and slightly inferiorly tilted had a significantly quicker onset of VF defects. The authors of this paper suggested that this was because of the uneven distribution of the retinal ganglion cell (RGC) axons, with more located in the macular area that is slightly inferior and temporal to the nerve.
The limitations of this study include its retrospective cohort design, as well as the non-inclusion of other parameters that may affect disease progression. In addition, the three-year follow-up period is short, considering that glaucoma is a chronic eye condition.
Nevertheless, the results of the study validate the conclusion that when predicting VF progression in patients with untreated NTG and myopia, the age of the patient and the disc morphology should also be evaluated.
Han, J., Han, S., Park, Y., Lee, E., & Kee, C. (2019). Clinical Course and Risk Factors for Visual Field Progression in Normal-Tension Glaucoma with Myopia without Glaucoma Medications. American Journal of Ophthalmology. doi: 10.1016/j.ajo.2019.08.023